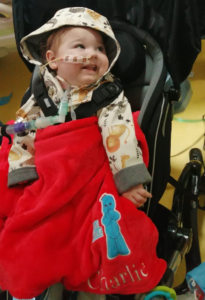
Charlie and Thomas
Charlie and Thomas
First published: 2nd September 2020
Charlie was born on the evening of the 19th September 2018, following a dramatic birth; upon delivery he had to be intubated, with copious amounts of meconium removed from his little body and then placed on CPAP.
After a three-day admission on SCBU, he was transferred to the ward with further tests and examinations carried out to ensure he was safe to be discharged home.
 Three days later, we were on our way home, proudly walking out with our baby boy. We noticed very quickly that he was feeding in a very peculiar way and that he was suffering from Colic, unlike we’d seen before in our previous children. Different bottles, various Colic syrups and a change of feed failed to have any significant impact. In the proceeding months, with many visits to the GP, formula changes, additives and more bottle changes, we weaned him onto baby food to settle down his reflux. It now became regular two hour stints each feed with Charlie suffering from severe discomfort during and after every feed.
Three days later, we were on our way home, proudly walking out with our baby boy. We noticed very quickly that he was feeding in a very peculiar way and that he was suffering from Colic, unlike we’d seen before in our previous children. Different bottles, various Colic syrups and a change of feed failed to have any significant impact. In the proceeding months, with many visits to the GP, formula changes, additives and more bottle changes, we weaned him onto baby food to settle down his reflux. It now became regular two hour stints each feed with Charlie suffering from severe discomfort during and after every feed.
Around five months we noticed a reduction of mobility and more milestones not being met, so after further visits to the GP and a visit to a Paediatric Consultant, it was agreed that if Charlie hadn’t seen any improvements an MRI scan would be ordered.
May 1st, 2019, I received a phone call from Sarah, Charlie’s mum, who was hysterical telling me he’d choked on a biscuit and he was receiving CPR. Later that evening we had a visit from a Dr, that informed us that Charlie’s diaphragm was paralysed on the right side, and that he’d expected to find changes when an MRI of Charlie’s brain was undertaken. This is the first time that we’d had our concerns a Cerebral palsy type of brain injury may have occurred at some point.
We were home for two nights. I took Charlie to A&E, as I suspected he had pneumonia, during an examination, Charlie got very agitated, then proceeded to have a huge desaturation to around 30% SpO2, he got agitated again then had a further desaturation to the low teens; this was unusual and he was readmitted back onto the children’s ward.
On the 24th May Charlie was transferred to hospital for examinations and an MRI, which confirmed that he had a Hypoxic-Ischemic Encephalopathy (HIE) brain injury.
Admitted onto the ward, Charlie now started having regular desaturations. Also, his reflux became a life-threatening event, Gastroesophageal Reflux, with most days having multiple of these episodes.
Charlie went to theatre for a fundoplication and a jej-peg feeding tube, to try and stop the life-threatening reflux. Charlie had a bed booked in PICU as a precaution, post op recovery, he had a big de-saturation and thus he stayed in PICU. After a week of multiple tests, Charlie was really struggling after a CT scan and had to be intubated and placed on a mechanical ventilator. Charlie had multiple trips to theatre and had an operation to plicate his diaphragm, during this operation his surgeon discovered a congenital diaghpramatic hernia! This is why Charlie used to struggle with his feeding so much, the poor boy, must have been in agony.
We found out in August that Sarah was pregnant with Thomas. After multiple failed extubations and Charlie’s pressures on his ventilator steadily increasing, concerns around ever getting off the vent were becoming apparent, following some very sudden loss of mobility after a viral infection, further Genetic testing was carried out and due to the pregnancy, this was urgent.
On November 8th I was called into the office as genetics had found something, it was SMARD1. I was told that this was progressive and ultimately fatal, usually by 13 months. Still reeling from the diagnosis, an urgent amniocentesis was ordered to check Thomas.
Following the amniocentesis, Sarah’s waters broke, at 16 weeks the prognosis was bleak. However, Thomas survived, only to be told five days later that he also had SMARD1 and given that when the waters break this early, this potentially results in significant damage to the respiratory system and other organs and would more likely be severely affected upon birth, even if the pregnancy made it through the next couple of weeks. Seeing how poorly Charlie was becoming, we made the heart breaking decision to end the pregnancy and not let Thomas suffer. Thomas was born sleeping, just under 18 weeks on the 28th November 2019 at 03:30. Around 15:00 I headed back over to the children’s hospital to be with Charlie in PICU.
 Surprisingly Charlie had gained more movement in his right arm and over the next few days further improvements and a respiratory stabilisation was occurring, and thus ensuring, we possibly had a bit more time with Charlie and enable him to enjoy positive experiences, which he achieved, mainly through his excellent consultant and the magnificent Claire House Children’s Hospice.
Surprisingly Charlie had gained more movement in his right arm and over the next few days further improvements and a respiratory stabilisation was occurring, and thus ensuring, we possibly had a bit more time with Charlie and enable him to enjoy positive experiences, which he achieved, mainly through his excellent consultant and the magnificent Claire House Children’s Hospice.
After months of continuous life and death decisions regarding Charlie’s care and saying right through when he started to suffer the severe effects of SMARD1, we’d act appropriately. The decision to withdraw care was taken on Friday 21st February with Charlie going to Claire House Children’s Hospice to pass away peacefully. We transferred Charlie on Monday 24th the February. We managed to get Charlie into the Hydrotherapy pool Monday and a trip to the Blue planet aquarium on Tuesday to give him a few more positives and fulfilled our "Bucket list" of positive experiences for Charlie, which Claire house made possible. Charlie passed away peacefully in our arms on 25th February 2020 around 9pm.
